Burn Severity in Prehospital Care: A Step-by-Step EMS Approach
Burn injuries can range from minor to life-threatening. For EMS clinicians, the ability to quickly assess burn severity in the field directly influences airway management, fluid resuscitation, destination decisions, and overall patient outcomes.
A strong burn assessment focuses on three core factors:
- Burn depth
- Total body surface area (TBSA) involved
- High-risk features that require specialty care
Understanding these elements allows EMS providers to recognize serious burns early and initiate the right treatment pathway.
Identify the Depth of the Burn
Burn depth helps determine how much tissue damage has occurred and how aggressively the patient may need to be managed.
Superficial burns affect only the outer skin layer, called the epidermis. These burns appear red and dry, similar to a mild sunburn. They blanch with pressure and typically do not blister. While painful, superficial burns usually heal without advanced medical treatment and do not count toward TBSA calculations used in severe burn management.
Partial-thickness burns extend into the dermis. These burns often appear red, moist, and blistered. They tend to be extremely painful because nerve endings remain intact. Partial-thickness burns do count toward TBSA when determining burn severity.
Full-thickness burns extend through the dermis and into deeper tissues. These burns may look white, brown, or charred. The skin often appears dry, leathery, and firm. Because nerve endings are destroyed, these burns may be less painful than partial-thickness injuries.
Recognizing these patterns allows EMS providers to estimate the seriousness of the injury even before advanced diagnostics are available.
Estimate Total Body Surface Area Quickly
Once you identify burn depth, the next step is to estimate the amount of skin involved.
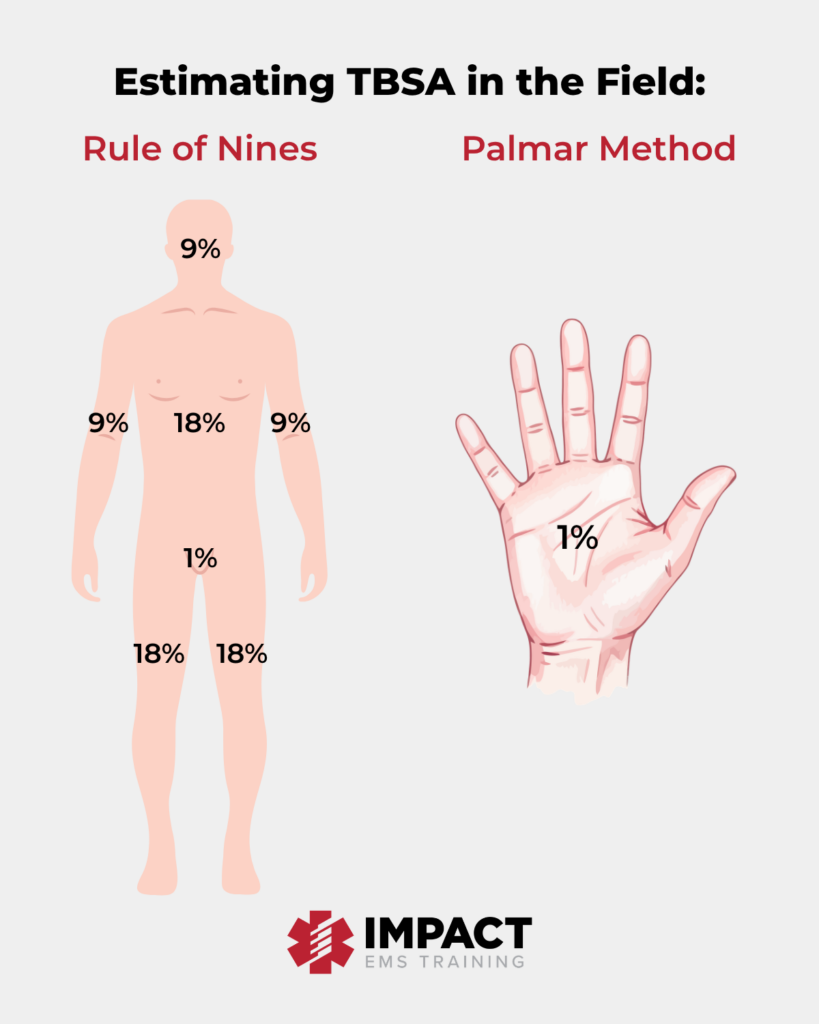
In adults, EMS providers often use the Rule of Nines to estimate TBSA in the field. This method divides the body into regions that represent roughly nine percent of the body’s surface area.
For example:
- Head and neck: 9%
- Each arm: 9%
- Each leg: 18%
- Anterior torso: 18%
- Posterior torso: 18%
- Perineum: 1%
For smaller burns, the Palmar Method can help. The patient’s palm, including the fingers, represent roughly 1 percent of TBSA.
Only partial-thickness and full-thickness burns count towards TBSA calculations for severe burns. Superficial burns are excluded.
Burns involving more than about 20 percent TBSA significantly increase the risk of systemic inflammation, fluid shifts, and burn shock. That threshold often marks the transition from a localized injury to a systemic emergency.
Look for Signs of Inhalation Injury
Burn severity is not limited to visible skin damage. Airway injury can rapidly complicate burn cases, especially in enclosed-space fires.
EMS providers should suspect inhalation injury when patients show:
- Burns to the face or neck
- Hoarseness or voice changes
- Soot in the mouth or nose
- Singed nasal hairs
- Exposure to smoke in an enclosed environment
- Altered mental status after a fire
These signs should raise concern for airway swelling or carbon monoxide exposure. Early airway management may be necessary before swelling progresses.
Recognize Burns that Require Specialty Care
Certain burns require rapid consultation with or transport to a burn center regardless of size.
These include burns involving:
- Face
- Hands
- Feet
- Genitalia or perineum
- Major joints
Other high-risk burns include:
- Electrical burns
- Chemical burns
- Lightning injuries
- Circumferential burns of the chest or extremities
- Burns combined with trauma
- Burns in patients with significant medical conditions
These injuries carry higher risks of complications, functional impairment, and long-term disability.
Apply a Systematic EMS Approach
In the prehospital setting, you should treat burn patients using the same structured approach you use for trauma patients.
A practical sequence includes:
- Address airway, breathing, and circulation first
- Estimate burn depth
- Calculates TBSA involvement
- Look for inhalation injury
- Identify high-risk burn patients
- Determine appropriate transport destination
Burn severity assessment does not require advanced technology. It requires careful observation, structured evaluation, and clinical judgment.
For EMS providers, mastering these fundamentals ensures burn patients receive the right care at the right time, starting from the moment the crew arrives on scene.
More from Impact EMS TRaining:
- Subscribe to Impact in Action to complete your Live CE license renewal requirements through interactive, cased based learning led by career EMS professionals.
- Advance your scope with Impact’s initial education, refresher, and test prep courses.
- Stay up to date with your state’s CE requirements.
- Review the Impact EMS Training Weekly Blog