
100% Silent
Chelsea Epling, BSN, RN, MCCN, EMT-P
I figured I’d start this one out with a disclosure. This is going to be more geared towards the nurses than it is toward the medics. Let’s face it, you all are just initially better trained on ventilators than we are.
Take a look at my experience. I started as a nurse working in a critical access emergency department. Limited resources mean you have to learn more skills because there isn’t always a designated person for every little task. This also meant that when we intubated a patient, our respiratory therapy heroes would be there to manage the vent until the helicopter or CCT ambulance arrived to take them to definitive care. The nurse was responsible for pushing RSI drugs, assessing EtCO2, lung sounds, etc., but the respiratory therapist handled the overall management of the ventilator.
Fast forward to my first few weeks in the ICU at a larger scale hospital. Almost every patient is on a ventilator. There’s one RT for the unit that often has to split their time between the unit and another floor. I’m given two patients to care for, for a full twelve-hour shift. During my orientation, one of the senior nurses said, “All you have to worry about are these two buttons: 100% and silent.” I’ve always had a curious mind and always wanted to learn more, even if it wasn’t technically solely “my responsibility.” Only knowing how to utilize two buttons didn’t sit well with me.
A few months after starting in the ICU, I was accepted into a flight training program. One of the big topics they discussed was how important it was to understand the ventilator, its functions, and how it plays a massive role in your patient’s overall well-being. Josh Pitrowski, ImpactEMS’s lead mechanical ventilation instructor (who you should really listen to if you get the chance), made a book for my training cohort specifically on the basics and fundamentals of ventilators and their functions. One thing he said that rang home for me was, “the ventilator can be the best thing for your patient when used appropriately; it can also be the most deadly when used incorrectly.” So here I was, a brand new ICU nurse, told that the only two things I needed to know were the 100% and the silent button, realizing that while my patient may be on multiple critical drips, a balloon pump or impella, or maybe even a ventriculostomy drain, the most dangerous thing my patient was connected to was the ventilator, of which its functions I had very little knowledge. I knew my goal was to eventually become a flight nurse, and I’d one day be responsible for managing a vent independently. I wasn’t sure where to start since this isn’t exactly a topic covered in nursing school…
…NURSES, THIS IS WHERE YOU FIND A SKILLED RT AND MAKE HIM YOUR BEST FRIEND. If you’re already working prehospital, your medic partner should be a good “vent guru” you can learn from as well. I read multiple books, watched countless YouTube videos, and listened to podcasts but still wasn’t fully understanding. I’m very much a hands-on learner and needed to physically get my hands on a vent to understand how it functioned. Thankfully, I worked with some of the most intelligent and skilled respiratory therapists around. They were more than happy to teach me anything and everything I needed to know about these machines. Today, my goal is to simply give you the basics, what you NEED to know if you’re caring for a patient on a mechanical ventilator.
VOLUME CONTROL VS PRESSURE
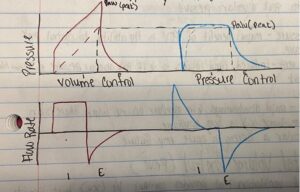
(The ICU Book, 2014)
VOLUME CONTROL
- Volume for this patient is preselected.
- The inflation volume is constant.
- The lungs are inflated with this ventilation mode at a constant flow rate, until the preset desired volume is delivered.
ADVANTAGES
- The patient will always get the desired volume with each breath.
- If airway resistance increases or lung compliance decreases, the ventilator generates a higher pressure to ensure adequate volume. This allows the ventilator to maintain the desired minute ventilation (rate [f] X volume [Vt]) when sudden or undetected changes occur.
DISADVANTAGES
- Airway pressure and the end of inspiration will be higher than that of a pressure control ventilation. This can be mistakenly diagnosed as ventilator-induced lung injury (VILI).
- The duration of inspiration is short, which can lead to uneven alveolar filling.
- There is a limited inspiratory flow, which can sometimes not meet the need of patients with high flow demands.
PRESSURE CONTROL
- The inflation pressure is preselected.
- A decelerating inspiratory flow rate provides high flows at the onset of lung inflation. This is to ensure that inflation pressures are obtained quickly.
- Inspiratory time is adjusted to allow enough time for the inspiratory flow rate to fall back to zero at the end of inspiration.
- Inspiratory airway pressure is the equivalent of peak alveolar pressure, so there is no airflow at the end inspiration.
ADVANTAGES
- You can control peak alveolar pressure. If peak alveolar pressure is 30cm H2O or less, there is a decreased risk of ventilator-induced lung injuries.
- This mode can be more comfortable for patients.
DISADVANTAGES
- There is a significant disadvantage in decreased alveolar volume when accompanied by increased airway resistance or decreased lung compliance.
- BIG CONCERN for patients in acute respiratory failure.
BASIC MODES OF MECHANICAL VENTILATION
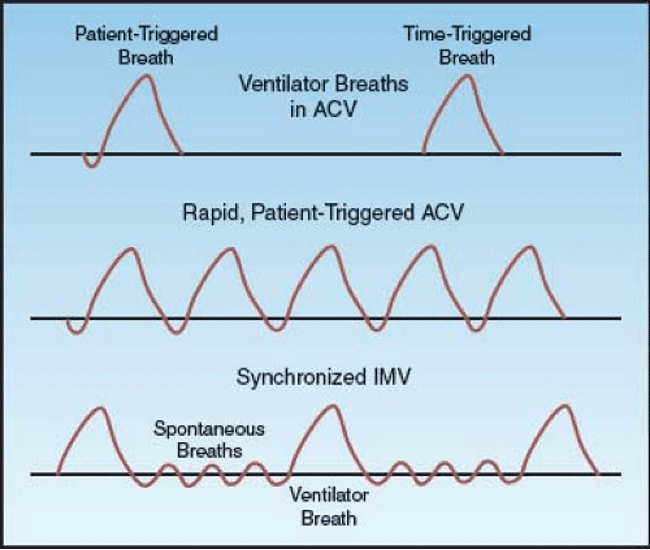
(The ICU Book, 2014)
A small explanation of the picture above. This image was taken from “Marino’sThe ICU Book,” which I highly recommend to anyone, nurse, medic, RT, physician, etc. that will be dealing with critically ill patients. The first illustration is of a patient taking regularly timed, volume-controlled breaths in assist-control mode. The second illustration shows a patient breathing at a rapid rate in assist-control mode, receiving the same volume with every breath. The third illustration shows a patient receiving the set volume for the set rate but pulling a lesser volume for the breaths taken above the ventilator setting in SIMV mode.
ASSIST-CONTROL (AC)
(Gentile, 2011).
I’m going to use as close to laymen’s terms as I can to break down these modes of ventilation. Assist-control ensures that the patient will breathe at the set rate and receive a preset Vt with each breath. If the patient takes a spontaneous breath or is breathing over the set rate, the patient will again receive that full set volume. This can become problematic if the patient is breathing too rapidly. It can severely decrease exhalation time and increase the risk for incomplete alveolar emptying and intrinsic PEEP. There are several reasons a patient may be breathing rapidly, such as inadequate sedation, pain, discomfort, or a physiological problem. If these have all been addressed and the patient continues to have rapid respirations, the patient should be switched from AC to SIMV (discussed in the next section.)
Referring back to the image above, there are two types of breaths shown in the first illustration. The waveform on the left shows a negative deflection, which will be seen when a patient takes a spontaneous breath. The waveform on the right, without a negative deflection, is triggered by the ventilator and shows no spontaneous inspiratory effort by the patient.
Synchronized Intermittent Mandatory Ventilation (SIMV)
(Kumar, 2020).
SIMV is a personal favorite of mine, especially in the prehospital/transport world. SIMV allows the patient to have spontaneous breaths but only delivers the full preset volume on the fixed set rate. If the patient is breathing above the ventilator, they only pull what volume their lungs allow. Occasionally in the transport environment, turbulence, a bump in the road, or any sudden movement may cause the ventilator to trigger, which could cause complications when left in AC mode. A significant indication for using SIMV is rapid breathing with incomplete exhalation during AC. This mode of ventilation allows for alveolar emptying and decreases the risk of air trapping and intrinsic PEEP. This mode of ventilation should be used cautiously, if at all, with patients with left-sided heart failure or weak respiratory muscles.
While there are many other modes of ventilation, including Pressure Support, often used when trying to wean the patient from the ventilator, those are the main settings you’ll see used in most EDs, ICUs, and transport/prehospital.
PEEP
One last thing I feel is essential to touch base on is PEEP. PEEP or positive end-expiratory pressure is significant in mechanically ventilated patients. PEEP is what keeps your alveoli open and prevents your lungs from collapsing. The amount of PEEP or lack thereof depends on the disease process. For example, a person with severe ARDS should typically have a much higher PEEP than a person with asthma, who may have no PEEP. As I stated earlier, I’m a hands-on learner, so PEEP didn’t connect with me until I could get my hands on a set of pig lungs and connect them to the ventilator. Without PEEP, your lungs collapse between breaths. With PEEP, they deflate on exhalation, but not completely. This is why, if your patient is on PEEP, especially high PEEP, you MUST clamp the ET tube before switching from BVM to ventilator or from the hospital vent to the transport vent.
The thing is, just because you’re a nurse, or in a hospital setting, or even if you’re part of a transport team fortunate enough to have their own RT, it DOES NOT mean that you don’t have to have a good understanding of what this machine’s capabilities. You need to be familiar with what a good waveform should look like. Are they breath stacking, are they asynchronous with the vent, are they not pulling enough volume, etc. Ultimately this should be part of your regular assessment of the ventilated patient. Good ventilator management can save a patient’s life. Poor ventilator management can kill them. It is your duty not to remain 100% silent. It is your duty to care for every aspect of your patient, ventilator included.
REFERENCES
Enrico, B., Cristian, F., Stefano, B., & Luigi, P. (2018). Patient-ventilator asynchronies: Types, outcomes, and nursing detection skills. ACTA Biomedica. doi:10.23750/abm.v89i7-S.7737
Gentile, M. A. (2011). Cycling of the mechanical ventilator breath. Respiratory Care. 56(1), 52-60. Doi: 10.4187/respcare.01088
Kumar, A. (2020). Synchronized intermittent mandatory ventilation (SIMV). Retrieved from https://embed online.com/airway/simv
Marino, P. L. (2014). Marino’s The ICU BOOK (4th ed.). New York, NY: Wolters Kluwer Health/Lippincott Williams & Wilkins.
Owens, W. (2012). The Ventilator Book. First Draught Press MMXII



